Response to How Low (Carb) Should You Go?
First of all, the recommendations I made were for a carbohydrate amount considerably higher than I currently follow or think is necessary for many people. While I don’t have the time or inclination to go point by point over every statement made, there are a few things I’d like to address:
1. Grains and/or starchy vegetables are not necessary to ensure adequate micronutrient intake.
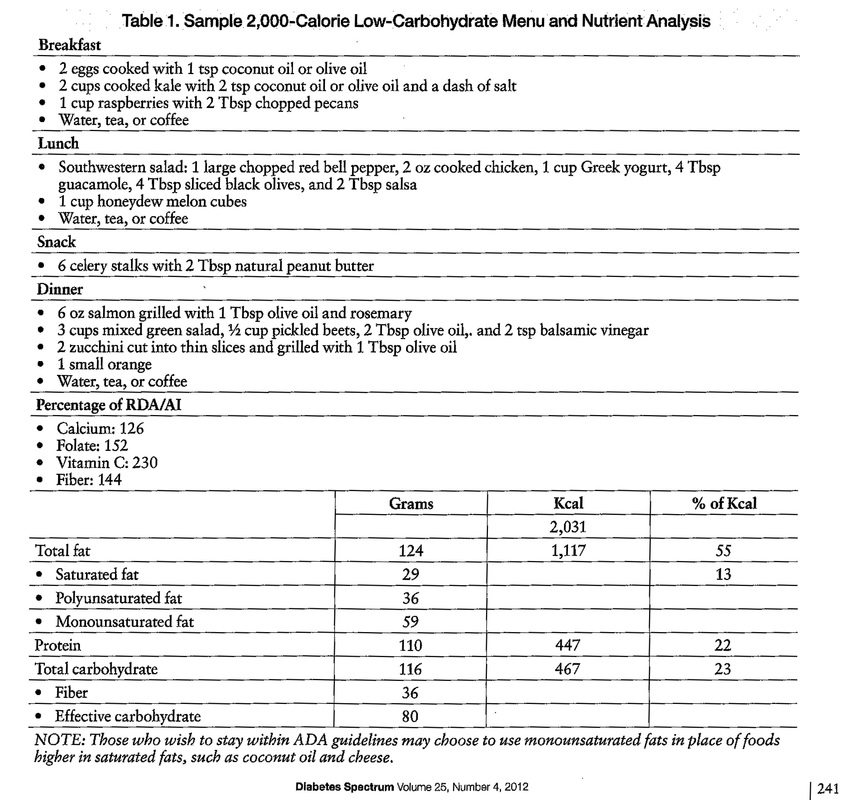
The post included my table containing a sample day’s menus and nutrient analysis for select vitamins and minerals. Space considerations did not permit me to list additional nutrients or calorie counts (I originally submitted four tables with different menus and calorie counts but was told I could choose only one).
Thiamin: 81%
Riboflavin: 164%
Niacin: 173%
Yes, the day was a little low on thiamin. Pork is the best source of thiamin, but I’m not necessarily suggesting people eat it every day. However, by slightly increasing the amount of nuts or animal protein, a person would easily meet the RDA . Also, consider the 10 Best Sources of Thiamin. Not a grain or starchy vegetable among them!
2. The fat content of this menu may be “elevated beyond the culinary comfort of most Americans,” but that doesn’t mean it is unhealthy or that a higher-fat diet would be difficult to adapt to.
I’ve discussed the issue of dietary fat in a previous blog post, and I have several references in my Diabetes Spectrum article regarding the lack of evidence that a high-fat diet contributes to heart disease or has other detrimental effects on health; on the contrary, such a diet may have a beneficial effect on lipid profiles and markers of inflammation. I believe a person with diabetes or metabolic syndrome following a “healthy, low-fat diet” that includes a breakfast such as a bowl of cereal with a banana and skim milk would achieve better blood sugar control and experience increased satiety by switching to the breakfast in the menu above and eating similar high-fat, moderate-protein, low-carb meals on a daily basis. This can be a very luxurious and satisfying way of eating.
3. Some people may find low carb difficult to stick to, but that doesn’t mean it shouldn’t be offered as an option for those who are interested in following it.
There is a well-known study indicating that a carb-restricted diet can be sustained over two years, but most studies are of much shorter duration. Unfortunately, the most difficult part of low carb is often at the beginning, when a person becomes adapted to using fat rather than glucose as a primary fuel source. There are many examples online of low-carb adherents — including doctors, nurses, dietitians, and other healthcare professionals — who have experienced great improvements in glycemic control and/or weight and find this way of eating enjoyable, energizing, and sustainable. I am one of them, and I will continue to advocate carbohydrate restriction as an alternative to the low-fat diet, higher-carbohydrate diets currently promoted by the majority of nutrition professionals.

I am so glad I found your link on fb .
Thank you, Barb!
It is going to take a very long time for the tide to finally change. The “low fat” mantra is too totally ingrained in the American psyche.
As of July 2013, I will have been consuming 20 net grams a day for 5 years, feel great, weight is finally under control after many, many years. Stopped taking statins, even though my doctor had a fit. I treadmill and do strength training 6 days a week. Life is good!
Thanks so much for sharing your fantastic results, Linda! So glad to hear success stories like yours.
Good for you, Franziska. I know you will stick to your guns. You had the courage to enter their “den of iniquity” (a little strong, perhaps), and I admire your commitment to continuing to do what you know is best. Isn’t it ironic that you modified your program somewhat, perhaps in the hope of gaining their acceptance and approval, and all they could do was pick at the corners and the details that publication did not allow you to include. Don’t be discouraged. You (and all of those who think as you do) have a growing audience. Frankly, I think they must feel threatened (and maybe even confused by the thought that they may be wrong!)
Dan, thank you so much for your feedback and continued support. It can be hard to keep speaking out when the voice of opposition comes from esteemed organizations like Joslin, but I can’t back down when I know how beneficial low carb can be from personal experience and that of others.
I know what you mean about Joslin, but their orientation stems from helping Type 1s, for whom a major object is to avoid hypos, so they are ‘conservative.’ Of course, Dr. Richard K. Bernstein wrote the book, literally, on how to do that using his concept of “small numbers.” Have you read his “Diabetes Solution”?
By the way, I wrote a column (#44) one year ago tomorrow about Joslin. It is now the 8th most popular in terms of page views on my blog. The link is http://www.thenutritiondebate.com/2012/03/nutrition-debate-44-joslin-clinic.html
Yes, I’ve read Diabetes Solution and refer to it regularly. Essential reading for anyone interested in achieving great BG control with low carb.
Thanks for the link to the Joslin article. Will try to read it later today.
You are my hero!!
You’re too kind, Linda. Thank you!
Well put, Franziska. I agree with you.
One of the reasons we always recommend for folks to get plenty of variety in their diets is so they don’t develop micronutrient deficiencies by always eating the same eight or 10 foods day after day. Coming in a little low on a micronutrient every now and then – like thiamin above – is not a problem.
Thanks, Steve. Agree that not always meeting 100% of the RDA for a vitamin or mineral isn’t a big deal. I just wanted to demonstrate that starchy carbs aren’t required, as needs can be met very well with low-carb foods.
Franziska, I am sickened every time the latest addition of Dietetics Today (UK) comes through my door!! It is little more than an advert for Kellogg’s… totally disheartening.
Good for you for speaking out, and taking your stand 🙂 I totally echo what Dan said above. They perhaps feel threatened, it really is a very confusing place to be to think you have been wrong about something for years. Looking back I was the same, but you need to get over it and start doing your own research, rather than blindly shelling out dated advice to patients who really need us to be real with them.
Thanks, Melanie. Agree that it’s really hard to admit that you may have been giving less-than-helpful advice to people for years. I have to remind myself that I didn’t always hold these beliefs and looked unfavorably at Atkins and other low-carb diets because I was taught they were unhealthy and unsustainable. It’s very encouraging to find out that open-minded RDs like you are also questioning standard dietary recommendations.
Just wanted to let you know I left a comment at the Joslin blog and they were gracious to publish it:
http://blog.joslin.org/2013/01/how-low-carb-should-you-go/
-Steve
Thanks so much, Steve. Appreciate your response, and happy to see that it was published.
I also applaud your honesty & integrity. Takes moxie to say the emperor has no clothes on. Weary, so weary, of hearing about the alleged deficiencies of LC & the praises sung of grains. Yes, that entire food group should be eliminated. The weak Joslin acknowledgement LC may be beneficial for some, followed by it’s something most can’t adhere to, is infuriating. Thank you, Joslin, ADA, CDA, et al, for gate-keeping & assuming what people can & cannot do.
Hopefully in the not too distant future LC will be accepted. Professionals like you are makig inroads & I’m grateful.
Thank you very much for your comments and support, Gerri. I’m actually pretty optimistic about low carb being considered a realistic option in the near future but completely understand your frustration. Appreciate your continued support.
Franziska,
I posted a comment on the Joslin blog that reviewed your article. It’s awaiting moderation but I thought I’d post it here too:
I congratulate Ms. Spritzler for credibly shedding some light on the value of a low carbohydrate diet. I have lived with Type 1 diabetes for 29 years. Eleven months ago I received a medical diagnosis of a significant diabetes complication. I was diagnosed T1D at the age of 30 and have maintained pretty good control on my blood glucose levels with most A1c’s in the 6% range. I did suffer a few years, however, some A1c’s as high as 8.5%. I fingerstick test about 15 times per day and use a continuous glucose monitor 24/7. I am very aware of how certain foods affect my postprandial blood glucose levels.
Subsequent to my recent diabetes complication diagnosis, I adopted a low carbohydrate diet (50-70 grams/day). The benefits to my health have been amazing! While my need for insulin dropped in half, my control markedly improved. My A1c dropped from 6.8% to 6.1% while hypoglycemia incidents fell from 2-3 per day to 2-3 per week. My glucose variability as measured by standard deviation went from 60 to 30.
I also lost 20 pounds and stopped taking blood pressure meds because my blood pressure normalized. I have more energy than before and feel emotionally and physically better.
I know that my story can easily be discarded as anecdotal, but the significant improvements to my health during the last 11 months are dramatic. I will never return to unhealthy high carb, low fat diet that I used for most of my adult life. Many argue that low carb eating is not sustainable. I’m here to tell you that I feel satiated and healthy eating as I do. I do not see any impediments to sustaining this way of eating.
From my vantage point, I see a medical/nutritional establishment is stuck in low fat/high carb “groupthink.” The past advice of a few dietitians over my 29 year diabetes career has not served me well. I encourage Joslin and other diabetes advocates to open their mind to a way of eating that is not only healthier but also sustainable.
Terry,
Thank you so much for sharing your story, and congratulations on all you’ve accomplished over the past year. I love hearing from people with T1 diabetes who experience improvements in A1c, less frequent hypoglycemic episodes, lower insulin requirements, and other health benefits on a highly palatable low-carb diet. Thanks also for posting at the Joslin website as well. I’m truly encouraged that someday soon carbohydrate restriction will be viewed as an acceptable — dare I say preferred — option for diabetes and weight control.
Hi Franziska,
“Ms. Spritzler does something medical researchers almost never do—she gives an example of a real world meal based on a carbohydrate load of approximately 20% of calories.”
Kudos!
I also agree that education is critical – a patient needs to know why they are being prescribed a specific dietary pattern: is it due to convenience, or because it is the best diet for their condition? If this distinction isn’t made, then many type II’s will mistakenly believe the high carb low fat diet they were told to eat is their best option.
all best,
Bill
Thanks so much, Bill! That’s my goal: to offer low carb as the best option for anyone with diabetes, metabolic syndrome, PCOS, and other conditions without fear of reprimand.
Everyone, please check out Bill’s blog, Calories Proper. Great stuff!
I hope you don’t mind me responding to your older blogs……they are new to me. I just sent your link to 2 more people. Anyway,
Franziska, you must truly know what salmon feel like trying to swim upstream through the dams of mainstream dietetics and big food. We have been so indoctrinated that we can’t see through the lies.
A conversation I had recently, at lunch with colleagues, is a perfect example: I overheard the words lo-carb said in a conversation at a different table. My ears perked up and I asked if that was what was said and one of my healthy weight colleagues said that his family is lo-carb so we started talking. Another person said “well I have to have my honey bunches of oats for breakfast,” as she rested her hands on her “wheat belly”. When I cringed, thinking about the poison she eats to start her day, another person who is dealing with health issues that would probably be solved by a lo-carb diet, asked “so what did you have for breakfast?” I told her that I had an omelet with cheese, chorizo, and fresh tomatoes.
She immediately said “so egg whites” and I said, “no, see that illustrates exactly what we have been talking about “big food “ and the way we have been so brainwashed.” Ya let’s throw out the most nutritious part of the egg…………………as I had been doing for 14 years……………and have a big bowl of heart healthy sugar grains. Sheeeesh
Please keep on swimming!
Of course I don’t mind, Rick. I appreciate your interest and support. Thanks for your comments and your insight.
I threw away egg yolks for years as well. Such a waste!